ED Approach to Dizziness
BPPV
AVS-acute vestibular syndrome
Treatment Article (Walker MF Treatment of Vestibular Neuritis)
quick phase nystagmus towards the intact ear)
treat with steroid taper similar to Bell’s palsy
(Stroke 2009;40:XX Kattah JC)
Head Impulse
horizontal head impulse test is a measure of the (VOR) vestibulo-ocular reflex
normal VOR=central
abnormal leans towards AVS, but does not rule-out central
Nystagmus
AVS should be associated with horizontal nystagmus that beats predominantly in one direction and increases in intensity when the patient looks in the direction of the fast phase. vertical nystagmus = central cause
Test of Skew
vertical ocular misalignment
Ocular tilt reaction=skew deviation, head tilt, and ocular counterroll
test with alt cover
tell pt to look straight ahead
cover eyes alternately
will see skewed eye move
long tract signs-
ED Folks conflate peripheral causes of dizziness
(Acad Emerg Med 2009;16:970)
BPPV-short lived less than a minute
article claims suppressants do not work
APV-may be more prevalent in the ED population, continuous dizziness lasting days to weeks. Even when a single spell, lasts hours.
should get steroids and suppressants (H1, Anticholinergics, Promethazines, Benzos)
The physical examination should focus on the systems that are involved in postural control and dizziness. Because the only objective sign of vertigo is nystagmus, examination of the eyes is extremely important in evaluating the dizzy patient. The general physical examination is often unrewarding in the dizzy patient. Possible etiologic clues include pressure asymmetry; orthostatic blood pressure change; cardiac irregularities; ear, nose, and throat abnormalities; head or neck bruit; abnormal range of neck motion; congenital abnormalities; or the stigmata of other illness that may cause dizziness.
The primary utility of the general neurologic evaluation is in looking for other indications or clinical signs that imply brain stem or other central nervous system sources for the patient’s complaints. Signs of abnormal central nervous system origin are most often found in examination of the cranial nerves. Mental status examination may give evidence of psychiatric or cognitive difficulties, which may affect the quality of the subjective data obtained from the patient. The Romberg has traditionally been considered a test of proprioceptive function. If this is negative, performing the sharpened Romberg may reveal subtle balance deficiencies undetectable with the ordinary Romberg test, especially in patients with acoustic tumors. A sharpened Romberg test is performed by having the patient place the heel of one foot to the toe of the other, with arms folded and eyes closed. Normal individuals should be able to stand in this position for longer than 30 seconds without significant sway.
Observation of the patient’s gait during the examination may reveal signs of unsteadiness, staggering, or a broad-based stance during walking. Additionally, one may get a sense of how well the patient is able to function.
The eyes should be carefully observed, preferably in a subdued light, for the presence of nystagmus. Vestibular nystagmus typically consists of a horizontal-rotatory, jerky motion with a slow and a fast component. Nystagmus that is equally rapid in both directions is not vestibular in origin. True vestibular nystagmus should also be suppressed by fixation of the gaze, convergence of the eyes, or gazing in the direction of the slow phase. Vertical nystagmus is never seen in vestibular disorders, whereas nystagmus in which the eyes wander or oscillate is often ocular in nature and may be related to a congenital disorder.
Ménière’s Syndrome
Ménière’s syndrome presents with a symptom constellation of aural fullness, fluctuating sensorineural hearing loss, tinnitus, and vertigo. The attack of vertigo reaches a maximal intensity within minutes of its onset then slowly subsides over the next several hours. The patient is usually left with a sense of unsteadiness and dizziness after the acute episode. In most cases, the patient is able to localize the symptom to the involved ear because of the associated hearing-related symptoms. In the early stages, the sensorineural hearing loss is in the low frequencies and is completely reversible, but in later stages a residual hearing loss remains and may involve both the middle and the high frequencies. The episodes may occur at irregular intervals for years, with periods of remission unpredictably intermixed. Eventually the syndrome reaches a burned-out phase, resulting in significant permanent hearing loss but a cessation of the vertigo.
Ménière’s syndrome is, by definition, idiopathic. Multiple causes have been suspected, including allergy, an autoimmune disorder, viral infection, and hormonal effects.8 The pathologic correlate is an excessive accumulation of endolymph, resulting in hydrops. As the volume of the endolymph increases, the membranous labyrinth expands and ruptures, resulting in hearing loss and vertigo.19
The treatment is largely aimed at preventing osmotic shifts in the endolymph. Medications, including vasodilator therapy and diuretics, are helpful for many patients.28 Patients are empirically placed on a low-sodium diet and asked to restrict caffeine and smoking. Specific treatment of any underlying allergies with immunotherapy or dietary avoidance of offending food allergens is also recommended. In a minority of cases, medical treatment is insufficient to control the episodes of vertigo, necessitating a surgical procedure. An endolymphatic mastoid shunt may be placed in the endolymphatic sac to decompress excess endolymph, or a selective sectioning of the vestibular nerve may be performed. In cases in which vertigo is disabling and there is no longer any useful hearing, a labyrinthectomy, with destruction of the neural elements, results in an effective control of vertigo.
The most prominent symptoms of tumors in the brain stem are hearing loss and tinnitus, rather than vertigo. Acoustic neuromas are benign schwannomas of the vestibular nerve sheath and are the most common cerebellopontine angle tumor. The vertigo associated with acoustic neuromas is usually mild or may even be absent: The slow growth rate of the tumor allows for central compensation. An acute attack of vertigo may be precipitated by a sudden swelling or hemorrhage of the tumor with brain stem compression. Other than eighth nerve dysfunction, the earliest neurologic sign in these patients is the loss of the corneal reflex.34 The diagnostic test of choice when the history or audiometric or other findings suggest this diagnosis would be a magnetic resonance imaging scan with gadolinium enhancement. The treatment is surgical removal of the tumor.
CPPV
from small cerebellar hemorrhage adjacent to the vermis
looks just like BPPV except may have direction changing nystagmus
Signs of Vestibular Neuritis
- Spontaneous, unidirectional, horizontal nystagmus is the most important physical finding.
- Fast phase oscillations beat toward the healthy ear.
- Nystagmus may be positional and apparent only when gazing toward the healthy ear, or during Hallpike maneuvers.
- Patients may suppress their nystagmus by visual fixation.
- Patient tends to fall toward his or her affected side when attempting ambulation or during Romberg tests.
- Affected side has either unilaterally impaired or no response to caloric stimulation.
- Vestibular neuronitis is unlikely if any of the following findings are present. The following symptoms should be absent:
- Multidirectional, nonfatiguing nystagmus suggesting vertigo of central origin
- Hearing loss
- Other cranial nerve deficits
- Truncal ataxia (suggests cerebellar disease or another CNS process)
- Inflamed tympanic membrane
- Mastoid tenderness
- High fever
- Nuchal rigidity
Isolated dizziness was associated with only 0.7% (9 of 1297) rate of stroke/tia. Imbalance with dizziness as referent was more likely to be stroke (Stroke 2006;37:2484)
BPPV
AVS-acute vestibular syndrome
Treatment Article (Walker MF Treatment of Vestibular Neuritis)
quick phase nystagmus towards the intact ear)
treat with steroid taper similar to Bell’s palsy
(Stroke 2009;40:XX Kattah JC)
Head Impulse
horizontal head impulse test is a measure of the (VOR) vestibulo-ocular reflex
normal VOR=central
abnormal leans towards AVS, but does not rule-out central
Nystagmus
AVS should be associated with horizontal nystagmus that beats predominantly in one direction and increases in intensity when the patient looks in the direction of the fast phase. vertical nystagmus = central cause
beats in one direction, worse when looking in the direction of the fast phase the fast phase is towards the good earworse when looking away from bad ear and towards good ear (Alexanders Law)if patient’s eyes are centered on nose and you turn to the patient’s right, and it causes catch-up then the right ear is the affected ear
Test of Skew
vertical ocular misalignment
Ocular tilt reaction=skew deviation, head tilt, and ocular counterroll
test with alt cover
tell pt to look straight ahead
cover eyes alternately
will see skewed eye move
long tract signs-
ED Folks conflate peripheral causes of dizziness
(Acad Emerg Med 2009;16:970)
BPPV-short lived less than a minute
article claims suppressants do not work
APV-may be more prevalent in the ED population, continuous dizziness lasting days to weeks. Even when a single spell, lasts hours.
should get steroids and suppressants (H1, Anticholinergics, Promethazines, Benzos)
The physical examination should focus on the systems that are involved in postural control and dizziness. Because the only objective sign of vertigo is nystagmus, examination of the eyes is extremely important in evaluating the dizzy patient. The general physical examination is often unrewarding in the dizzy patient. Possible etiologic clues include pressure asymmetry; orthostatic blood pressure change; cardiac irregularities; ear, nose, and throat abnormalities; head or neck bruit; abnormal range of neck motion; congenital abnormalities; or the stigmata of other illness that may cause dizziness.
The primary utility of the general neurologic evaluation is in looking for other indications or clinical signs that imply brain stem or other central nervous system sources for the patient’s complaints. Signs of abnormal central nervous system origin are most often found in examination of the cranial nerves. Mental status examination may give evidence of psychiatric or cognitive difficulties, which may affect the quality of the subjective data obtained from the patient. The Romberg has traditionally been considered a test of proprioceptive function. If this is negative, performing the sharpened Romberg may reveal subtle balance deficiencies undetectable with the ordinary Romberg test, especially in patients with acoustic tumors. A sharpened Romberg test is performed by having the patient place the heel of one foot to the toe of the other, with arms folded and eyes closed. Normal individuals should be able to stand in this position for longer than 30 seconds without significant sway.
Observation of the patient’s gait during the examination may reveal signs of unsteadiness, staggering, or a broad-based stance during walking. Additionally, one may get a sense of how well the patient is able to function.
The eyes should be carefully observed, preferably in a subdued light, for the presence of nystagmus. Vestibular nystagmus typically consists of a horizontal-rotatory, jerky motion with a slow and a fast component. Nystagmus that is equally rapid in both directions is not vestibular in origin. True vestibular nystagmus should also be suppressed by fixation of the gaze, convergence of the eyes, or gazing in the direction of the slow phase. Vertical nystagmus is never seen in vestibular disorders, whereas nystagmus in which the eyes wander or oscillate is often ocular in nature and may be related to a congenital disorder.
Ménière’s Syndrome
Ménière’s syndrome presents with a symptom constellation of aural fullness, fluctuating sensorineural hearing loss, tinnitus, and vertigo. The attack of vertigo reaches a maximal intensity within minutes of its onset then slowly subsides over the next several hours. The patient is usually left with a sense of unsteadiness and dizziness after the acute episode. In most cases, the patient is able to localize the symptom to the involved ear because of the associated hearing-related symptoms. In the early stages, the sensorineural hearing loss is in the low frequencies and is completely reversible, but in later stages a residual hearing loss remains and may involve both the middle and the high frequencies. The episodes may occur at irregular intervals for years, with periods of remission unpredictably intermixed. Eventually the syndrome reaches a burned-out phase, resulting in significant permanent hearing loss but a cessation of the vertigo.
Ménière’s syndrome is, by definition, idiopathic. Multiple causes have been suspected, including allergy, an autoimmune disorder, viral infection, and hormonal effects.8 The pathologic correlate is an excessive accumulation of endolymph, resulting in hydrops. As the volume of the endolymph increases, the membranous labyrinth expands and ruptures, resulting in hearing loss and vertigo.19
The treatment is largely aimed at preventing osmotic shifts in the endolymph. Medications, including vasodilator therapy and diuretics, are helpful for many patients.28 Patients are empirically placed on a low-sodium diet and asked to restrict caffeine and smoking. Specific treatment of any underlying allergies with immunotherapy or dietary avoidance of offending food allergens is also recommended. In a minority of cases, medical treatment is insufficient to control the episodes of vertigo, necessitating a surgical procedure. An endolymphatic mastoid shunt may be placed in the endolymphatic sac to decompress excess endolymph, or a selective sectioning of the vestibular nerve may be performed. In cases in which vertigo is disabling and there is no longer any useful hearing, a labyrinthectomy, with destruction of the neural elements, results in an effective control of vertigo.
The most prominent symptoms of tumors in the brain stem are hearing loss and tinnitus, rather than vertigo. Acoustic neuromas are benign schwannomas of the vestibular nerve sheath and are the most common cerebellopontine angle tumor. The vertigo associated with acoustic neuromas is usually mild or may even be absent: The slow growth rate of the tumor allows for central compensation. An acute attack of vertigo may be precipitated by a sudden swelling or hemorrhage of the tumor with brain stem compression. Other than eighth nerve dysfunction, the earliest neurologic sign in these patients is the loss of the corneal reflex.34 The diagnostic test of choice when the history or audiometric or other findings suggest this diagnosis would be a magnetic resonance imaging scan with gadolinium enhancement. The treatment is surgical removal of the tumor.
CPPV
from small cerebellar hemorrhage adjacent to the vermis
looks just like BPPV except may have direction changing nystagmus
Signs of Vestibular Neuritis
- Spontaneous, unidirectional, horizontal nystagmus is the most important physical finding.
- Fast phase oscillations beat toward the healthy ear.
- Nystagmus may be positional and apparent only when gazing toward the healthy ear, or during Hallpike maneuvers.
- Patients may suppress their nystagmus by visual fixation.
- Patient tends to fall toward his or her affected side when attempting ambulation or during Romberg tests.
- Affected side has either unilaterally impaired or no response to caloric stimulation.
- Vestibular neuronitis is unlikely if any of the following findings are present. The following symptoms should be absent:
- Multidirectional, nonfatiguing nystagmus suggesting vertigo of central origin
- Hearing loss
- Other cranial nerve deficits
- Truncal ataxia (suggests cerebellar disease or another CNS process)
- Inflamed tympanic membrane
- Mastoid tenderness
- High fever
- Nuchal rigidity
Isolated dizziness was associated with only 0.7% (9 of 1297) rate of stroke/tia. Imbalance with dizziness as referent was more likely to be stroke (Stroke 2006;37:2484)
The Dizzy Patient
Essential Elements Of The History
Is true vertigo present?
What is the pattern of onset?
What is the duration of the symptoms?
Have there been auditory symptoms?
Are there associated neurologic symptoms?
Are there other associated symptoms?
What is the patients past medical history?
What medications is the patient taking?
Semicircular ducts for angular acceleration of the head. Have three ducts with X, Y, Z axis. Semicircular canal is filled with fluid. Only work on acceleration so when at rest or moving at constant velocity, these are not active.
Utricle and saccule measure linear acceleration. Have otoliths to allow the system to be gravity sensitive F=ma, acceleration is the force of gravity, need the little grains of sand to satisfy the mass. Endolymph in the canals, perilymph around.
True vertigo is worse with the eyes shut.
Test nystagmus only a few degrees off center, not at extremes of vision. Vertical nystagmus will happen regardless of where the eyes are looking.
Academic Emergency Medicine Volume 10, Number 12 1388-1395,
Etiologies
Peripheral Causes
Foreign body in ear canal
Cerumen or hair against tympanic membrane
Acute otitis media
Labyrinthitis (suppurative, serous, toxic, chronic)
Benign positional vertigo
Ménières disease
Vestibular neuronitis (assoc with viral URIs)
Perilymphatic fistula
Trauma (labyrinth concussion)
Motion sickness
Acoustic neuroma *
Central Causes
Infection (encephalitis, meningitis, brain abscess)
Vertebral basilar artery insufficiency
Subclavian steal syndrome
Cerebellar hemorrhage or infarction
Vertebral basilar migraine
Posttraumatic injury (temporal bone fracture)
Postconcussive syndrome
Temporal lobe epilepsy
Tumor
Multiple sclerosis
Cervical spine muscle and ligamentous injury
Systemic Causes
Diabetes mellitus
Hypothyroidism
Many medications have direct vestibulotoxicity. The most commonly encountered are the aminoglycosides, anticonvulsants, alcohols, quinine, quinidine, and minocycline. In addition, caffeine and nicotine can have wide-ranging autonomic effects that may exacerbate vestibular symptoms. The history of past and present illnesses should be explored, with specific questioning about the existence of diabetes and drug or alcohol use.
Peripheral
sudden, severe, horizontal nystagmus (never vertical), worsened by position, assoc. auditory findings Thenystagmus seen with BPV shows latency; that is, its onset occursapproximately 10 seconds after the inciting movement and resolvesafter 30 to 60 seconds, when the vertigo resolves.
Central
gradual, mild, any type of nystagmus (vertical is always central) gaze directed (beats in direction of gaze) while peripheral will be direction fixed. Central nystagmus will stay present with gaze fixation. Central nystagmusdoes not fatigue and is not decreased by fixation
whisper similar sounding words into each ear, if can not discriminate words then problem of nerve itself (neuroma)
ACEP Lecture by Martin Samuels, MD
Never suggest words or symptom to the patient. Ask them exactly what is going on? Then keep repeating the last three words of what the patient has said, then pause, until hell freezes over or the patient gives you more. Listen to neighborhood symptoms (the symptoms will tell you what systems are near the patient’s complaints)
Divide into Four Categories
- Vertigo (Illusion (misperception of a stimulus) of hallucination (misperception without stimulus) of movement)
- Hallucinatory vertigo can be caused by migraine and epileptic (40%)
- Near-Syncope (Decreased cerebral perfusion) (30%)
- Ask if you have ever had this sensation when lying down
- Disequilibrium (Gait Disorder) (10%)
- Ill-defined lightheadedness (Anxiety) (20%)
Exam
- Make sure you examine the ear.
- Test Hearing:
- Hearing Loss?
- Is it sensory neural? (Rinne 256-512 mHz) Touch the mastoid or place in front of ear. Air should be better than bone. Test the first then the second, ask which one is better. If air is better then sensory neural.
- Is the problem cochlear or retrocochlear? Retrocochlear could be a Scwann cell vestibular neuroma (Get MRI, not emergent problem.)
- Look for Spontaneous Nystagmus while sitting with EOM testing
- Screening Neurological: Walk, talk, eyes, stand, babinski, visual fields.
Vertigo
- BPPV is the most common
- Perilymphatic fistula, usually from old injury reactivated by coughing, etc. Nystagmus caused by insufflating auditory canal and causing nystagmus.
- Labrynthitis and Vestibular Neuronitus: Bell’s Palsy of VIII, Give 5 days of steroid.
- Meniere’s Disease: Look for autoantibodies in blood, this form might respond to steroids, otherwise treat symptomatically.
- Traumatic Vertigo: after major trauma, usually resolves spontaneously in 6-8 weeks.
- Vestibular Neuroma
Near Syncope
Ambient circumstance. Temperature, drugs, etoh, or anxiety leading to hyperventilation.
Disequilibrium
extrapyramidal symptoms
cervical spondylosis decreases proprioception. Worse in the shower b/c the shower is a Romberg machine
Peripheral neuropathy: destroys proprioception
Myelopathy
B12 Deficiency
Anxiety
Will just keep repeating dizzy no matter how many times you ask for another word.
Tell them they have Type IV dizziness.
Use anticholinergic drug that penetrates the BBB, benadryl or meclizine (only antihistamines that have anticholinergic side effects 50 mg po q4-6)
Can give atropine to young people 0.5-1 mg
Use Phenergan for nausea
Avoid scopolamine b/c of side effects
Methylphenidate to reverse the drowsiness
Benzos are only for type IV dizziness. If you are going to use a benzo, use only short acting.
NASA uses meclizine and methylphenidate with great success.
Cerebellar TIA or Stroke
Review Article to diff peripheral from cerebellar
For patients with a history of recurrentvertigo, in whom TIA is a consideration, the duration (minutes)helps to distinguish TIA from BPV, which lasts seconds, andMeniere’s disease, which lasts hours. In addition, the onsetof central vertigo is spontaneous, whereas that of BPV is clearlyassociated with sudden changes in position of the head. Tinnitusand hearing loss are unusual in patients with posterior circulationinfarcts. Patients with vestibular neuritis and labyrinthitisand patients with stroke have prolonged vertigo. Vertigo associatedwith labyrinthitis or neuritis comes on slowly over hours, whereasthat associated with a cerebrovascular accident begins suddenly.The nystagmus that accompanies peripheral disorders remits after24 to 48 hours, but the central nystagmus persists. In addition,infarction of brainstem vestibular structures or the cerebellumis typically accompanied by neighborhood signs.
Neighborhood signs
lateralizingcerebellar findings Eye findings or cerebellar testing disorders
Purely vertical or bidirectional nystagmusis associated with central lesions
Vertebral/Basilar insufficiency
think of in elderly with 1st onset vertigo
ISOLATED ACUTE VERTIGO IN THE ELDERLY: VESTIBULAR OR VASCULAR DISEASE? Norrving, B., et al, Acta Neurol Scand 91(1):43, January 1995 BACKGROUND: In elderly patients, acute vertigo accompanied by nystagmus, nausea and vomiting without other neurologic abnormalities (representing “isolated vertigo”) is frequently considered to be a benign and self-limiting condition not requiring extensive diagnostic evaluation. However, isolated vertigo may also be caused by potentially serious central pathology. METHODS: This prospective Swedish study examined findings in 24 patients aged 50-75 with apparent acute “isolated vertigo” in the absence of previous vestibular symptoms or history of transient ischemic attack or stroke. The patients were evaluated with MRI (22 cases) or acute-phase CT scanning (two cases), in addition to electro-oculography and Doppler studies of the vertebral, basilar, carotid and peri-orbital arteries. RESULTS: Infarcts of the caudal cerebellum were diagnosed in six patients (25%). Potential cardioembolic sources were identified in three of these six, and Doppler studies demonstrated ipsilateral vertebral artery occlusion in the remaining three. Cerebellar infarctions were characteristically associated with ataxic pursuit eye movements on electro-oculography (noted in four of six cases). On follow-up which ranged from 3-33 months after initial presentation (median, 24.5 months), eight patients had been placed on either anticoagulants (two) or aspirin (six). One patient with an initially normal MRI but unilateral vertebral artery occlusion on Doppler sonography had experienced a stroke (representing an annual incidence of 2.5%). CONCLUSIONS: Cerebellar infarctions may be responsible for signs and symptoms in about one-fourth of patients presenting with apparent acute isolated vertigo. Clinical assessment and caloric testing alone may result in misdiagnosis.
If the patient presents in the early fall wearing a red vest and one leather glove, the diagnosis is obvious. “Bow hunters stroke” consists of repeated vertebrobasilar ischemic attacks induced by head rotation 45º to the left, as when shooting an arrow.
Other causes include chiropractic manipulation, yoga, and cervical trauma. Even a vigorous shampoo in hyperextended neck position can produce cervical vertigoproviding a compelling argument for washing your own hair.
I would like to point out three potential physical diagnostic signs of cerebellar infarction with isolated vertigo. First, Lee et al studied patients with cerebellar infarction presenting with isolated vertigo (vestibular pseudoneuritis), and found that 56 percent had direction-changing nystagmus. (Neurology 2006;67:1178.) Secondly, the same team found that 71 percent of such patients had the inability to walk without support.Although the patient with vestibular neuritis may have a staggering gait, most patients with an intact central nervous system retain the ability to walk. These signs are not new and have been advocated in review articles from the New England Journal of Medicine. (1998;339:680.)
More recently, Cnyrim (J Neurol Neurosurg Psychiatry 2008;79:458) found that skew deviation was present in 40 percent of patients with vestibular pseudoneuritis but no patients with vestibular neuritis. This study included all central mimics of vestibular neuritis, but cerebellar infarction was prominent among them. Skew deviation is a type of vertical misalignment of the eyes that can be caused by cerebellar damage as well as other conditions. Any vertical malalignment of the eyes, whether subjectively reported as vertical diplopia or objectively observed on ocular movement examination, should be considered potentially worrisome for cerebellar infarction.
While I grant that derangements of gait and ocular movement are already part of a seasoned clinician’s examination, these specific findings probably deserve to be outlined so that the readers will recognize these signs with greater accuracy and confidence. Clinicians should specifically look for direction-changing nystagmus, the inability to walk without support, and skew deviation as potential physical signs of cerebellar infarction in the patient with acute isolated vertigo and no localizing neurologic deficits. – James A. Nelson, MD, San Diego
Normal head impulse test (Neurology 2008;70:2378) Acute peripheral vestibulopathy (APV) with hearing involvement=labrynthitis without=vestibular neuritis — + HIT = abnormal vesibular-ocular reflex had 100% specificity and 91% sensitivity normal = +; abnormal = negative recent trauma; think dissection inferior cerebellar strokes are pseudo-labrynthine nystagmus named by the rapid movement HIT is rapid passive head rotation while the patient keeps their eyes fixed on your nose negative f they can stay focused abnormal if they can’t when you rotate their head to the side of the nerve dysfunction
Wallenbergs Syndrome
Occlusion of the PICA (Posterior Inferior Cerebral Artery)
Loss of pain/temp on ipsilateral face and contra body. Ataxia. Vertigo
Menieres
vertigo, tinnitus, hearing loss
Multiple Sclerosis
CN III is weak, VI normal when looking to side
Test nystagmus both stationery and positional.
Benign Positional Vertigo
episodes last a few minutes, assoc c specific head position
Patients with BPPV have very brief (5-30 seconds) episodes of vertigo. However they will not infrequently say that their dizziness is all the time because theyre left with a vague sense of somethings not right in between episodes. You need to carefully tease this out by history.
usually caused by canalith or otolith which escapes the saccule and usually goes into posterior canal.
Vertigo with rotary nystagmus. Should reverse on upright posture. Lasts for~60 seconds. Eventually CNS figures out what’s going on and fatigues the response.
Jogging, bending over, hitting brake in car can all be provocative.
Provocative test
Hallpike-Dix.
Have pt sit up, then lay quickly supine, turn head to the side of ear being tested, ~45º and extend neck 30° off horizontal, repeat on other side
Nystagmus usually occurs within 10 seconds after positioning but may present as late as 40 seconds. Hence, if the history is classic, observe the patient for at least 40 seconds while he or she is in the head-hanging position during the Hallpike test.
Head-thrust test (HTT)
was first described in 1988 in alaboratory study of 12 patients with unilateral section of thevestibular nerve for acoustic neuroma or intractable vertigo.All 12 patients had a discernibly abnormal test result. TheHTT is conducted by having the patient fixate on the examiner’snose, with the head turned horizontally 10° to 20° offthe midline. The examiner turns the patient’s head rapidly backto the midline and observes the eye movements. The normal responseis for the eyes to remain fixated on the examiner’s face, movingsmoothly to keep up with the head rotation. If there is a unilateralvestibular deficit, when the head is turned in the directionof the defective ear, the eyes make discernible saccades, orjumps, back to the target to compensate for the slowed reflexresponse to the head turn. These saccades may also be observedin infarction of the area of the brainstem at the origin ofthe eighth nerve; however, in that case other brainstem findingsare invariably present.16,17 The HTT has been subsequently evaluatedin several studies of patients with known unilateral vestibularloss and shown to be highly sensitive but has not been thoroughlystudied in patients with central causes of vertigo to determineits specificity.18,19 As a simple bedside test that may adduseful information in the attempt to identify peripheral lesions,its utility in the ED setting deserves further study.
Therapeutic Maneuver
Do it on every + Hallpike, huge benefit. (Chang Acad Emerg Med 2004;11:918)
Epley maneuver for canalith repositioning:
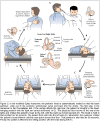
Fig. 1. Epley maneuver. Top (left to right), The first window is a legend for the inset, which is a simplified representation of a posterior semicircular canal. This figure shows the Epley canalith-repositioning maneuver for the left semicircular canal. The patients head is turned 45 degrees toward the affected ear, with the patient holding the physicians arm for support. The patient is then lowered to a supine position. The patients head remains turned 45 degrees and should hang off the end of the bed. Bottom, In the third position, the patient s head is rotated to face the opposite shoulder. Next, the patient is rolled onto his or her side, taking care to keep the head rotated. The patient is now returned to a seated position with the head tilted forward.
The Key is to wait 30 seconds or until complete resolution of symptoms between each position change
http://www.emedicine.com/emerg/topic57.htm
place to get movies
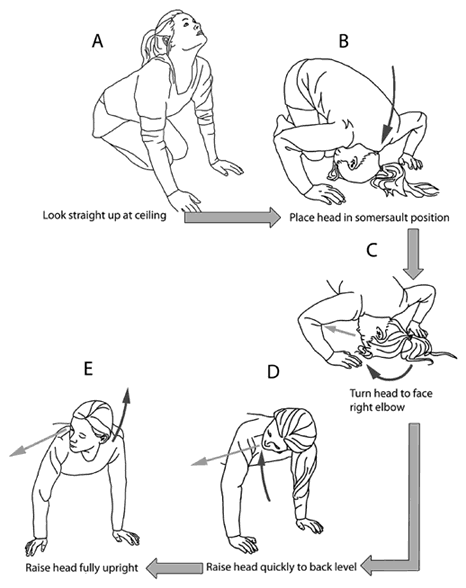
Half-Somersault
Brandt-Daroff exercises
for benign paroxysmal positional vertigo. The patient should be advised to perform these movements in both directions twice daily. Each time they are performed the patient should move in each direction three times, i.e., left ear down and back to seated, then right ear down and back to seated, then again left ear down and back to seated, and so forth. Reprinted from
(Arch Otolaryngol. 1980;106:484-5.)
Intravenous Lorazepam versus dimenhydrinate for treatment of vertigo in the emergency department: a randomized clinical trial. Our results suggest that dimenhydrinate was more effective in relieving vertigo and less sedating than lorazepam at the intravenous doses administered in this study. Dimenhydrinate appears to be the preferred medicine for patients who present to the ED with vertigo likely to be of peripheral origin. (Ann Emerg Med. 2000 Oct;36(4):310-9.)
Labyrinthitis
Vertigo, nystagmus, tinnitus, hearing loss, can be toxic or infectious
Vestibular Neuronitis
sudden attack last hours then subsides gradually, no hearing effects
BPV
Symptoms of BPV are usually worse in the morning (the otoliths are more likely to clump together as the patient sleeps and exert a greater effect when the patient gets up in the morning) and mitigate as the day progresses (the otoliths become more dispersed with head movement). Nausea is typically present (vomiting is less common). A history of head trauma may be present, especially in young patients with BPV. The head trauma may dislodge the otoliths off their membrane within the utricle, allowing them the opportunity to enter the semicircular canals. Eliciting that the individual episodes of vertigo in BPV last for seconds at a time is important. Patients may describe that they are having continuous vertigo, when in reality, they are having repeated episodes (with each episode lasting less than a minute). Patients with vestibular neuritis and labyrinthitis have continuous vertigo, often for hours to days. This author asks the patient if the room is spinning during the interview (while the patient’s head is still and prior to any manipulative tests). If the patient states that he or she is currently symptomatic, then it is highly unlikely that the patient has BPV because the vertigo in BPV lasts for seconds at a time and occurs only after head movement.
Jeff Mann
perform a complete neurological examination including all the following observations:-
- mental status
- cranial nerves
- sensorimotor exam of the limbs
- speech evaluation for dysarthria and/or dysphonia
- swallowing assessment for dysphagia
- finger-nose and heel-knee testing for dysmetria
- rapid hand movement testing for dysdiadochokinesis (fine motor coordination)
- gaze preferences at rest
- whether the eyes move conjugatedly in all directions of gaze without overshoot/undershoot phenomena and secondary corrective step-oscillations (saccadic testing)
- smoothness of visual pursuit eye movements (using your moving finger as a visual target in all directions of gaze)
- visual acuity and confrontational visual fields
- presence of a Horner’s syndrome
checking for gait ataxia(= getting the patient to stand and then evaluating the patient’s ability to walk) is a critical part of the neurological examination
- a patient with acute vestibular ataxia is very disinclined to walk, but the patient can usually walk if strongly ecouraged/coaxed to walk
- a patient with acute vestibular ataxia has a tendency to list or fall or veer or stagger towards the affected side
- a patient with acute vestibular ataxia has a greater inability to maintain his balance when standing or walking with the eyes closed, because of the loss of visual cues that can counterbalance the vestibular impairment (* perform an enhanced Romberg test by asking the patient to stand upright with the eyes closed => then ask the patient to march on the spot => the patient will tend to rotate towards the side of the lesion – called a positive Fukuda or Unterberger test)
- a patient with acute cerebellar ataxia due to a cerebellar/brain stem stroke may have extreme truncal ataxia and a total inability to stand or even take a single step without falling, and there is no definite tendency to tilt or fall to any particular side => an ED physician may mistakenly conclude that the patient will not walk, when he cannot walk
- however, a patient with acute cerebellar ataxia may occasionally only have mild truncal ataxia that is unaffected by closing the eyes, and subtle truncal ataxia (slight unsteadiness when turning around or changing direction) may be difficult to differentiate from the poor balance found in patients with severe peripheral vertigo
- may disappear temporarily after repeating the maneuver several times
Differentiating between central and peripheral paroxysmal positional nystagmus Appearance Latentcy Duration Fatigability Localisation Central Pure vertical, usually downbeat Unusual Persistent Unusual Brainstem or cerebellum PeripheralTorsional upbeat or horizontal geotropic Usual Brief Usual Posterior or horizontal semi-circular canal
– vertigo and nystagmus may also be induced in a patient with BPV affecting the horizontal semi-circular canals by suddenly turning the patient’s head to the affected side while the patient is lying supine in the horizontal position and observing for induced vertigo +/- nystagmus => the nystagmus is horizontal, appears after a latent period of 1 – 10 seconds, and disappears after 1 minute with occasional reversal of the nystagmus prior to resolution
Evaluation of nystagmus in a patient with vertigo
– it is important to clearly understand the effect of visual fixation on nystagmus testing, because many cases of nystagmus may be missed or misinterpreted if testing for nystagmus is only performed using “visual fixation techniques” eg. asking the patient to fixate on the examiner’s finger and instructing the patient to follow the finger as it is moved from side-to-side
– it is important to check for nystagmus not only when the patient is fixating, but also when he is not fixating, so that you do not miss subtle clues differentiating peripheral from central vertigo
Example number 1 – when the nystagmus is present in primary gaze, and in both directions of gaze
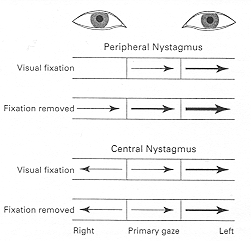
– the direction of the fast phase of the nystagmus is indicated by the direction of the arrows, and the intensity of the nystagmus is represented by the thickness of the arrows
– in peripheral vertigo, the direction of nystagmus is always in the same direction even if the direction of gaze changes from left-to-right, while in central vertigo the direction of the nystagmus can change direction when looking in the opposite direction
– also note that in peripheral vertigo that the intensity of the nystagmus increases when visual fixation is removed, while the intensity of the nystgamus in central vertigo is relatively unaffected by visual fixation
Example number 2 – when the nystagmus is only present in one direction of gaze
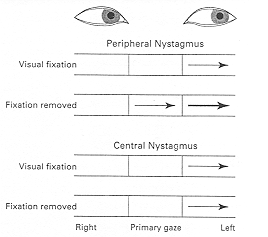
– note that there is no difference in the direction of the nystagmus, or the intensity of the nystagmus, when the patient is visually fixating – whether the cause of the nystagmus is peripheral or central
– note that the only clue to peripheral vertigo can be a slight increase in the intensity of the nystagmus when the patient is not visually fixating
– is is therefore very important to repeat testing for nystagmus using non-visual fixation techniques (fresnel lenses or darkened room + patient vaguely staring into the distance when instructed to look to the left and then to the right) to detect any subtle change in intensity of the nystagmus – a subtle increase in the intensity of the nystagmus when the patient is not visually fixating may be the only clue differentiating peripheral from central vertigo eg. inferior cerebellar infarct
Summary of the clinical features differentiating acute peripheral vestibular syndrome from acute central vestibular syndrome Peripheral Central Onset of vertigo Sudden/gradual Sudden/Gradual Severity of vertigo Often intense and disabling Less distinct and disabling Pattern of vertigo Paroxysmal, constant, waxing-and-waning Constant Vertigo aggravated by head or body movement/position Yes No Associated nausea, vomiting, diaphoresis Frequent and prominent Infrequent and less severe Nystagmus type Horizontal or torsional; or mixed horizonto-torsional, but never vertical or horizontal Horizontal, torsional or vertical Nystagmus direction Unidirectional with fast phase always away from the affected ear (irrespective of direction of gaze) May be bidirectional, and may change direction with changes in direction of gaze Nystagmus intensity affected by fixation Intensity decreased or totally suppressed by visual fixation Intensity unaffected by visual fixation Nystagmus intensity affected by direction of gaze Nystagmus intensity may be increased when looking in direction of fast phase Nystagmus intensity is usually unaffected by direction of gaze Nystagmus fatiguability Nystagmus decreases or disappears with repeat testing Nytagmus remains prominent despite repeat testing Fatigue of vertigo symptoms over time Yes No Hearing loss May be present Very infrequent CNS symptoms/signs Absent Present GaitMild-moderate ataxia with tendency to fall towards one side – opposite to the direction of the fast phase of nystagmus Moderate-severe ataxia with inability to walk, or tendency to fall to either side
Epley maneuver – Canalith re-postioning maneuver
– this maneuver can be used to treat patients with benign paroxysmal positional vertigo (BPPV)
– the maneuver is based on the theory that benign paroxysmal positional vertigo (canalolithiasis) is due the sudden movement of free-floating particles (otoconia) that accumulate in the posterior semi-circular canal => sudden head movements (looking up, rolling over in bed, leaning forward) cause the debris to move about en masse in the posterior semi-circular canal => vertigo lasting a few seconds
– treatment of BPPV can be undertaken in the ED by performing the Epley maneuver as follows:-
– seat the patient upright on the bed with his head extending over the edge of the bed (as in the Dix-Hallpike maneuver test) => tilt the patient’s head gently 45 degrees towards the affected side => gently lower the head of the bed so that the patient is lying in the horizontal position with his head over the edge of the bed – his head should then be about 45 degrees below the horizontal level => wait about 30 – 60 seconds for the patient’s vertigo to subside, and then keep the patient in that position for ~ 3 minutes => turn the patient’s head gently to the midline => wait 30 seconds => turn the patient’s head another 45 degrees to the opposite (unaffected) side => wait 30 seconds => let the patient slowly roll his torso towards that opposite side so that he is lying on that opposite shoulder, which should enable him to rotate his head another 45 degrees in that opposite direction so that his face is directed towards the floor => wait 30 seconds for any induced vertigo to resolve and keep the patient in that position for ~ 3 minutes => slowly bring the patient back up to the vertical position while he is still lying in that position => then gently turn his head back towards the midline => when he is sitting upright, tilt the chin down about 30 degrees and keep the patient in that position for a few minutes
– if the patient is very vertiginous during the maneuver, anti-emetics may first have to be given in order to to successfully complete the maneuver
– the manuever may have to be repeated a few times and the patient should be told to sleep upright and minimize head movements during the next 24 – 48 hours; the patient should still expect to have a sense of dysequilibrium for a few days
– a clue to an unsuccessful canolith repositioning maneuver is nystagmus that changes direction during the maneuver (any nystagmus occurring during the maneuver should be in the same direction as the original nystagmus, which occurred when the patient was first placed flat with the affected ear undermost)
Drugs used in the outpatient treatment of acute peripheral vertigo Scopolamine – 0.5 mg transdermal patch qd Diphenhydramine – 25 – 50 mg qid Cyclizine – 25 – 50 mg qid Meclizine – 12.5 – 50mg tid Diazepam – 2.5 mg tid Flunarazine – 10mg qd
ED Approach to Dizziness
BPPV
AVS-acute vestibular syndrome
Treatment Article (Walker MF Treatment of Vestibular Neuritis)
quick phase nystagmus towards the intact ear)
treat with steroid taper similar to Bell’s palsy
(Stroke 2009;40:XX Kattah JC)
Head Impulse
horizontal head impulse test is a measure of the (VOR) vestibulo-ocular reflex
normal VOR=central
abnormal leans towards AVS, but does not rule-out central
Nystagmus
AVS should be associated with horizontal nystagmus that beats predominantly in one direction and increases in intensity when the patient looks in the direction of the fast phase. vertical nystagmus = central cause
Test of Skew
vertical ocular misalignment
Ocular tilt reaction=skew deviation, head tilt, and ocular counterroll
test with alt cover
tell pt to look straight ahead
cover eyes alternately
will see skewed eye move
long tract signs-
ED Folks conflate peripheral causes of dizziness
(Acad Emerg Med 2009;16:970)
BPPV-short lived less than a minute
article claims suppressants do not work
APV-may be more prevalent in the ED population, continuous dizziness lasting days to weeks. Even when a single spell, lasts hours.
should get steroids and suppressants (H1, Anticholinergics, Promethazines, Benzos)
The physical examination should focus on the systems that are involved in postural control and dizziness. Because the only objective sign of vertigo is nystagmus, examination of the eyes is extremely important in evaluating the dizzy patient. The general physical examination is often unrewarding in the dizzy patient. Possible etiologic clues include pressure asymmetry; orthostatic blood pressure change; cardiac irregularities; ear, nose, and throat abnormalities; head or neck bruit; abnormal range of neck motion; congenital abnormalities; or the stigmata of other illness that may cause dizziness.
The primary utility of the general neurologic evaluation is in looking for other indications or clinical signs that imply brain stem or other central nervous system sources for the patient’s complaints. Signs of abnormal central nervous system origin are most often found in examination of the cranial nerves. Mental status examination may give evidence of psychiatric or cognitive difficulties, which may affect the quality of the subjective data obtained from the patient. The Romberg has traditionally been considered a test of proprioceptive function. If this is negative, performing the sharpened Romberg may reveal subtle balance deficiencies undetectable with the ordinary Romberg test, especially in patients with acoustic tumors. A sharpened Romberg test is performed by having the patient place the heel of one foot to the toe of the other, with arms folded and eyes closed. Normal individuals should be able to stand in this position for longer than 30 seconds without significant sway.
Observation of the patient’s gait during the examination may reveal signs of unsteadiness, staggering, or a broad-based stance during walking. Additionally, one may get a sense of how well the patient is able to function.
The eyes should be carefully observed, preferably in a subdued light, for the presence of nystagmus. Vestibular nystagmus typically consists of a horizontal-rotatory, jerky motion with a slow and a fast component. Nystagmus that is equally rapid in both directions is not vestibular in origin. True vestibular nystagmus should also be suppressed by fixation of the gaze, convergence of the eyes, or gazing in the direction of the slow phase. Vertical nystagmus is never seen in vestibular disorders, whereas nystagmus in which the eyes wander or oscillate is often ocular in nature and may be related to a congenital disorder.
Ménière’s Syndrome
Ménière’s syndrome presents with a symptom constellation of aural fullness, fluctuating sensorineural hearing loss, tinnitus, and vertigo. The attack of vertigo reaches a maximal intensity within minutes of its onset then slowly subsides over the next several hours. The patient is usually left with a sense of unsteadiness and dizziness after the acute episode. In most cases, the patient is able to localize the symptom to the involved ear because of the associated hearing-related symptoms. In the early stages, the sensorineural hearing loss is in the low frequencies and is completely reversible, but in later stages a residual hearing loss remains and may involve both the middle and the high frequencies. The episodes may occur at irregular intervals for years, with periods of remission unpredictably intermixed. Eventually the syndrome reaches a burned-out phase, resulting in significant permanent hearing loss but a cessation of the vertigo.
Ménière’s syndrome is, by definition, idiopathic. Multiple causes have been suspected, including allergy, an autoimmune disorder, viral infection, and hormonal effects.8 The pathologic correlate is an excessive accumulation of endolymph, resulting in hydrops. As the volume of the endolymph increases, the membranous labyrinth expands and ruptures, resulting in hearing loss and vertigo.19
The treatment is largely aimed at preventing osmotic shifts in the endolymph. Medications, including vasodilator therapy and diuretics, are helpful for many patients.28 Patients are empirically placed on a low-sodium diet and asked to restrict caffeine and smoking. Specific treatment of any underlying allergies with immunotherapy or dietary avoidance of offending food allergens is also recommended. In a minority of cases, medical treatment is insufficient to control the episodes of vertigo, necessitating a surgical procedure. An endolymphatic mastoid shunt may be placed in the endolymphatic sac to decompress excess endolymph, or a selective sectioning of the vestibular nerve may be performed. In cases in which vertigo is disabling and there is no longer any useful hearing, a labyrinthectomy, with destruction of the neural elements, results in an effective control of vertigo.
The most prominent symptoms of tumors in the brain stem are hearing loss and tinnitus, rather than vertigo. Acoustic neuromas are benign schwannomas of the vestibular nerve sheath and are the most common cerebellopontine angle tumor. The vertigo associated with acoustic neuromas is usually mild or may even be absent: The slow growth rate of the tumor allows for central compensation. An acute attack of vertigo may be precipitated by a sudden swelling or hemorrhage of the tumor with brain stem compression. Other than eighth nerve dysfunction, the earliest neurologic sign in these patients is the loss of the corneal reflex.34 The diagnostic test of choice when the history or audiometric or other findings suggest this diagnosis would be a magnetic resonance imaging scan with gadolinium enhancement. The treatment is surgical removal of the tumor.
CPPV
from small cerebellar hemorrhage adjacent to the vermis
looks just like BPPV except may have direction changing nystagmus
Signs of Vestibular Neuritis
- Spontaneous, unidirectional, horizontal nystagmus is the most important physical finding.
- Fast phase oscillations beat toward the healthy ear.
- Nystagmus may be positional and apparent only when gazing toward the healthy ear, or during Hallpike maneuvers.
- Patients may suppress their nystagmus by visual fixation.
- Patient tends to fall toward his or her affected side when attempting ambulation or during Romberg tests.
- Affected side has either unilaterally impaired or no response to caloric stimulation.
- Vestibular neuronitis is unlikely if any of the following findings are present. The following symptoms should be absent:
- Multidirectional, nonfatiguing nystagmus suggesting vertigo of central origin
- Hearing loss
- Other cranial nerve deficits
- Truncal ataxia (suggests cerebellar disease or another CNS process)
- Inflamed tympanic membrane
- Mastoid tenderness
- High fever
- Nuchal rigidity
Isolated dizziness was associated with only 0.7% (9 of 1297) rate of stroke/tia. Imbalance with dizziness as referent was more likely to be stroke (Stroke 2006;37:2484)
| | |