Consider these in all patients with ABD Pn
AAA
Cardiac Ischemia
Mesenteric Ischemia
DKA
Hernia
Testicular Torsion/Ovarian Torsion
Nephrolithiasis
Porphyria
pain during first few days of menstrual cycle=endometriosis or endometrioma
Analgesics for Abdominal Pain
Surgeons review the literature (Am J Surg 185:291, April 2003)
1st Study: Ann R Coll Surg Engl 1986;68:209-210
2nd Study: BMJ 1992;305:554-6
3rd Study: Acad Emerg Med 1996;3:1086-92
4th Study: J Emerg Med 1997;15:775-9.
Not mentioned is: J Am Coll Surg. 2003 Jan;196(1):18-31, a prospective, double blind with 74 patients.
and Am J Emerg Med 18(7):753, November 2000, another small prospective randomized trial
largest trial to date shows ok to give (ann emerg med 2006;48:150)
rational clinical exam series (JAMA 2006;296(14):1764)
opiate admin had no signif. negative effects
Special Considerations
The Elderly
With each decade of life, mortality increases and diagnostic accuracy decreases. The risk of surgical pathology is much, much higher. (Scand J Gastroent 1988:144:35-42)
HIV
In addition to normal pathology, can also have bacterial enterocolitis, drug induced pancreatitis, or AIDS-related cholangiopathy.
Women of Child Bearing Age
Urinary vs. Gastrointestinal vs. Pelvic etiologies.
If women is pregnant, diff. becomes much wider. In 3rd trimester, the appendix will be in the extreme upper right quadrant.
High Yield Questions
- Which came first, the pain or the vomiting?
- How long have you had the pain (>48hrs is more reassuring.)
- Prior surgeries?
- Could you jump up and down right now?
- Are you taking any antibiotics or steroids?
- Do you have a history of hypertension, vascular problems, or A. Fib?
Abdominal Exam
Abdominal Contour should always be assessed
Carnett’s sign-increased tenderness to palpation when abdominal muscles are contracted (have pt raise their head or lift his legs)
Most appendices are inferior and medial to McBurney’s point. 20% of appies will have no RLQ pain or tenderness. Use cough test or heel drop (pt drops from standing on toes on to heels) or simply bang the heels to test for peritoneal signs.
Murphy’s Sign Sensitivity ~97% hold palpation of RUQ, have take deep breath. Place L hand with the index finger on the lowest rib with the thumb in the midclavicular line. Press thumb into the belly and have the patient take a deep breath. Repeat with placebo by doing the same with the thumb just touching the skin.
McBurney’s Point 1 1/2 – 2 inches from anterior spinous process of ilium on a straight line from that process to umbilicus
Psoas Sign specificity 95% flex thigh against resistance
Obdurator sign-rotate flexed thigh internally and externally
Rovsing sign-pain in RLQ with palpation of LLQ
Make pt take deep breath to differentiate between voluntary and involuntary guarding
All women with undifferentiated ABD pain should have a pelvic, PID can present as RUQ pain b/c of Fitz-Hugh-Curtis)
Pelvic Exam has very little sensitivity or specificity in females with abdominal pain if they are not pregnant (Canadian Journal of EM 5:2, March 2003)
Antibiotics
ABX: Amp or amp/gent. Unasyn 1.5 g proph or 3g
Rx If allergic: clinda/gent
or cipro/flagyl
Pneumoperitoneum
Pneumoperitoneum should resolve 2-3 days post-op on X-ray
Tension Pneumoperitoneum is a consequence of colonoscopy c perf. Relieve c 14 G just like paracentesis
Non-Abdominal causes of Abdominal Pain
Heme: Sickle Cell,
Metabolic
Porphyria
·
Increased production of porphobilinogen
·
“Port wine” urine
·
Precipitated by decreased heme production
·
Severe abdominal pain, very benign exam
·
Similar episodes in past
·
Asssociated with CNS changes
Categories to consider
·
Hematologic sickle cell, thrombocytosis, coagulopathies, leukemia, lymphoma
·
Metabolic – above
·
Infectious RMSF, TB, Varicella, meningococcemia, lyme disease
·
Inflammatory HSP, polyarteritis nodosa, vasculitis, SLE, eosinphilic enteritis
·
Toxin – black widow, heavy metal
·
Psychogenic somatization, munchhausen, malingering
Clues to suggest a systemic cause:
·
Diffuse pain
·
Pain out of proportion to exam
·
Patient sick, exam benign
·
Constitutional symptoms
·
Immunocompromised, Elderly
·
Multiple return visits
Test for porphyria
A fresh urine sample protected from light has been sent for Watson-Schwartz test [
H.L. Bonkowsky and G.F. Barnard, Diagnosis of porphyric syndromes: a practical approach in the era of molecular biology, Semin. Liver Dis. 18 (1998), pp. 5765.
Derivation of CPR (American Journal of Emergency Medicine (2005) 23, 709717)
showed that Non-contrast CT should be done on all pts as hist and phys is specific but not at all sensitive
Spontaneous Hemoperitineum
Spontaneous Hemoperitoneum (Emerg Radiol 2007;14:65)
ruptured ovarian cyst, ectopic, spont rupture of liver or hepatic mass, tumor, inflammation, endometriosis,
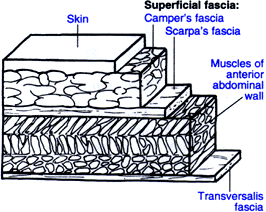
Abdominal Layers
The New EMedHome Clinical Pearl is: Chilaiditis Sign
Chilaiditis Sign
Chilaiditis sign (pronounced “Ky-La-Ditty”) refers to the usually asymptomatic interposition of the bowel (typically the hepatic flexure of the colon) between the liver and the (right) hemidiaphragm. The importance of this sign is that it can mimic the radiographic appearance of pneumoperitoneum.
Chilaiditi’s syndrome refers to this radiographic finding plus symptomatology. The “syndrome” may involve nausea, vomiting, abdominal pain, anorexia, constipation or respiratory distress. The clinical presentation of Chilaiditis syndrome may simulate pneumoperitoneum, even though it is a benign entity.
Identifying haustral folds between the liver and diaphragm can distinguish pneumoperitoneum from Chilaiditi syndrome. Furthermore, the radiographic findings of Chilaiditi’s sign on plain radiographs will not move with change in position, unlike pneumoperitoneum; a left lateral decubitus abdominal film may help in this distinction. If the distinction is still unclear, CT scan can be used to make the final diagnosis.
Click Here for a radiographic example of Chilaiditis sign.
References: (1) Lo BM. Radiographic Look-alikes: Distinguishing between Pneumoperitoneum and Pseudopneumoperitoneum. J Emerg Med. 2008; Aug 30 [Epub ahead of print]. (2) Sanyal K, Sabanathan K. Air below the right diaphragm: Chilaiditi sign. Emerg Med J. 2008;25: 300.
Spontaneous Retroperitoneal Hemorrhage
Retroperitoneal Hemorrhage from EMEDHome
Spontaneous retroperitoneal bleeding can present in the absence of specific underlying pathology or trauma and is commonly seen in association with anticoagulation therapy. Given the frequency of patients presenting to the ED on triple anticoagulant therapy (warfarin, aspirin, and clopidogrel), emergency physicians need to be aware that the presentation is varied and may be vague and that retroperitoneal hematomas can present as an acute femoral neuropathy. Early identification is crucial to improving patient morbidity and mortality.
Retroperitoneal hematomas can result in femoral neuropathy at 2 different locations along the femoral nerve’s course. The first is the iliopsoas gutter due to the rigid surrounding fascia. The second is at the inguinal ligament overlying the femoral canal, which contains the femoral nerve.
Femoral neuropathy caused by retroperitoneal hematoma may present with sudden onset severe pain in the affected groin and hip, with radiation to the anterior thigh and the lumbar region. Femoral neuropathy can result in quadriceps muscle weakness and the sensation of the knee buckling. Later on, pain and paresthesia in the anterior thigh is characteristic.
References:
(1) Krause, ML, et al. Mayo Clin Proc 2011; 86: e21-e24.
(2) Parmer SS, et al. Ann Vasc Surg 2006;20: 536-540.
(3) Sasson Z, et al. Can J Cardiol 1996; 12: 490-4.
| | |
